TANGIER DISEASE vs FAMILIAL HYPERCHOLESTEROLEMIA
A form 6 student share a news with you. “I am shocked when I look at my blood test result. My blood total cholesterol is more than 300 mg/dL, the LDL cholesterol is be more than 220 mg/dL, but my Triglyceride levels tend to be normal, which are below 150 mg/dL. I am still young! I have a healthy lifestyle because I do not want to be like my mother who is having hypercholesterol. Am I having Tangier’s disease?”.
Explain him the condition and things he can do to help himself. Explain what is Tangier’s disease too.
Explain him the condition and things he can do to help himself. Explain what is Tangier’s disease too.
What is Tangier disease?
Tangier disease is an inherited disorder characterized by significantly reduced levels of high-density lipoprotein (HDL) in the blood. HDL transports cholesterol and certain fats called phospholipids from the body's tissues to the liver, where they are removed from the blood. HDL is often referred to as "good cholesterol" because high levels of this substance reduce the chances of developing heart and blood vessel (cardiovascular) disease. Because people with Tangier disease have very low levels of HDL, they have a moderately increased risk of cardiovascular disease.
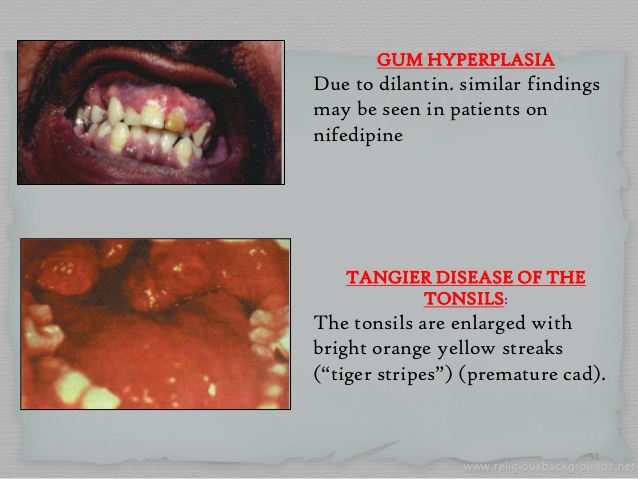
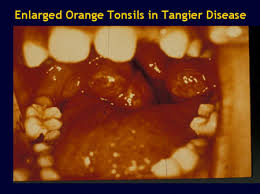
Additional signs and symptoms of Tangier disease include a slightly elevated amount of fat in the blood (mild hypertriglyceridemia); disturbances in nerve function (neuropathy); and enlarged, orange-colored tonsils. Affected individuals often develop atherosclerosis, which is an accumulation of fatty deposits and scar-like tissue in the lining of the arteries. Other features of this condition may include an enlarged spleen (splenomegaly), an enlarged liver (hepatomegaly), clouding of the clear covering of the eye (corneal clouding), and type 2 diabetes.
How common is Tangier disease?Tangier disease is a rare disorder with approximately 100 cases identified worldwide. More cases are likely undiagnosed. This condition is named after an island off the coast of Virginia where the first affected individuals were identified.
What genes are related to Tangier disease?
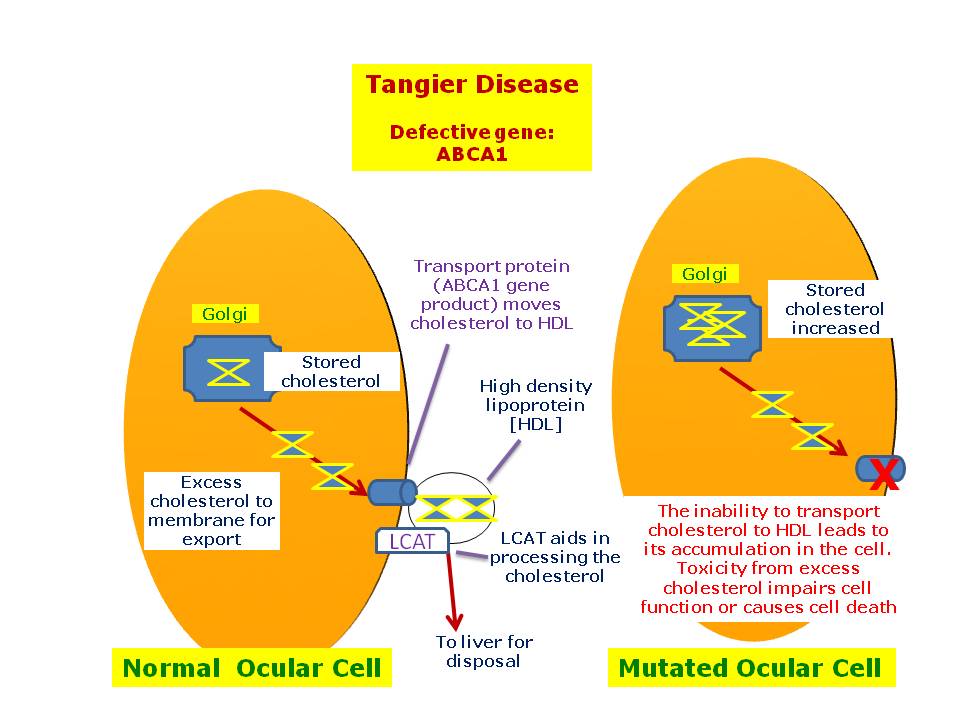
Mutations in the ABCA1 gene cause Tangier disease. This gene provides instructions for making a protein that releases cholesterol and phospholipids from cells. These substances are used to make HDL, which transports them to the liver.
Mutations in the ABCA1 gene prevent the release of cholesterol and phospholipids from cells. As a result, these substances accumulate within cells, causing certain body tissues to enlarge and the tonsils to acquire a yellowish-orange color. A buildup of cholesterol can be toxic to cells, leading to impaired cell function or cell death. In addition, the inability to transport cholesterol and phospholipids out of cells results in very low HDL levels, which increases the risk of cardiovascular disease. These combined factors cause the signs and symptoms of Tangier disease.
Read more about the ABCA1 gene.
How do people inherit Tangier disease?
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Tangier disease is an inherited disorder characterized by significantly reduced levels of high-density lipoprotein (HDL) in the blood. HDL transports cholesterol and certain fats called phospholipids from the body's tissues to the liver, where they are removed from the blood. HDL is often referred to as "good cholesterol" because high levels of this substance reduce the chances of developing heart and blood vessel (cardiovascular) disease. Because people with Tangier disease have very low levels of HDL, they have a moderately increased risk of cardiovascular disease.
Additional signs and symptoms of Tangier disease include a slightly elevated amount of fat in the blood (mild hypertriglyceridemia); disturbances in nerve function (neuropathy); and enlarged, orange-colored tonsils. Affected individuals often develop atherosclerosis, which is an accumulation of fatty deposits and scar-like tissue in the lining of the arteries. Other features of this condition may include an enlarged spleen (splenomegaly), an enlarged liver (hepatomegaly), clouding of the clear covering of the eye (corneal clouding), and type 2 diabetes.
How common is Tangier disease?Tangier disease is a rare disorder with approximately 100 cases identified worldwide. More cases are likely undiagnosed. This condition is named after an island off the coast of Virginia where the first affected individuals were identified.
What genes are related to Tangier disease?
Mutations in the ABCA1 gene cause Tangier disease. This gene provides instructions for making a protein that releases cholesterol and phospholipids from cells. These substances are used to make HDL, which transports them to the liver.
Mutations in the ABCA1 gene prevent the release of cholesterol and phospholipids from cells. As a result, these substances accumulate within cells, causing certain body tissues to enlarge and the tonsils to acquire a yellowish-orange color. A buildup of cholesterol can be toxic to cells, leading to impaired cell function or cell death. In addition, the inability to transport cholesterol and phospholipids out of cells results in very low HDL levels, which increases the risk of cardiovascular disease. These combined factors cause the signs and symptoms of Tangier disease.
Read more about the ABCA1 gene.
How do people inherit Tangier disease?
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
👉 Familial Hypercholesterolemia
Cholesterol plays a vital part in how our body works, but if levels get too high, it increases our risk of heart disease. For most of us, this doesn’t happen until we’re in our 40s, and a common cause is eating too much saturated fat in things like butter, cheese, cakes and pastries. So there’s a lot we can do to keep the levels under control, and we should all try to have a healthy lifestyle to reduce our risk of heart disease. But for some people, it’s not just a question of lifestyle and getting older. About one in 200 people has familial hypercholesterolaemia (FH), an inherited condition that means their cholesterol levels are higher than normal from birth. It’s caused by an abnormal gene and, despite it putting people at high risk of early heart disease, most of them don’t even know they have it.
What’s the difference between FH and standard high cholesterol?
Anyone can develop high cholesterol as they age, but FH is a genetic condition, passed on to you by one of your parents. When you have FH, your cholesterol is high from birth, whereas most people’s cholesterol goes up as they get older and they may be 50, 60 or 70 before their cholesterol is considered high enough to increase their risk of heart disease. So it’s not that the cholesterol itself is any different, but that your risk of heart disease is much higher because you’ve had high cholesterol for so much longer. Someone who is 40 with FH could easily have the heart attack risk of a 70 year old.
Anyone can develop high cholesterol as they age, but FH is a genetic condition, passed on to you by one of your parents. When you have FH, your cholesterol is high from birth, whereas most people’s cholesterol goes up as they get older and they may be 50, 60 or 70 before their cholesterol is considered high enough to increase their risk of heart disease. So it’s not that the cholesterol itself is any different, but that your risk of heart disease is much higher because you’ve had high cholesterol for so much longer. Someone who is 40 with FH could easily have the heart attack risk of a 70 year old.
What problems can FH cause?
If untreated, about 50 per cent of men and 30 per cent of women with FH will develop coronary heart disease by the time they’re 55
If untreated, about 50 per cent of men and 30 per cent of women with FH will develop coronary heart disease by the time they’re 55.
On average in the UK, one person a day with FH has a heart attack. About a third of people don’t survive their first heart attack, and many who do survive will have damaged hearts.
The good news is that a 2008 study part-funded by the BHF found that people with FH who are diagnosed and treated before they develop heart disease generally live as long as people who don’t have FH. So it’s really important to get diagnosed as early as possible.
If untreated, about 50 per cent of men and 30 per cent of women with FH will develop coronary heart disease by the time they’re 55
If untreated, about 50 per cent of men and 30 per cent of women with FH will develop coronary heart disease by the time they’re 55.
On average in the UK, one person a day with FH has a heart attack. About a third of people don’t survive their first heart attack, and many who do survive will have damaged hearts.
The good news is that a 2008 study part-funded by the BHF found that people with FH who are diagnosed and treated before they develop heart disease generally live as long as people who don’t have FH. So it’s really important to get diagnosed as early as possible.
How do I know if I have FH?
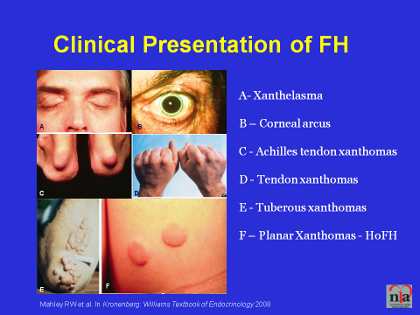
The classic signs of FH are lumps and bumps around your knuckles or Achilles tendon (caused by cholesterol deposits), yellow cholesterol build-up around the eyes and eyelids, or a pale ring around the iris of your eye.
The classic signs of FH are lumps and bumps around your knuckles or Achilles tendon (caused by cholesterol deposits), yellow cholesterol build-up around the eyes and eyelids, or a pale ring around the iris of your eye.

What can I do?
-Eat a healthy balanced diet that is low in saturated fat
-plenty of fresh fruit and vegetables
-Keeping fit and active will also help to keep your heart healthy and it’s essential that you don’t smoke.
-If you have FH, a healthy lifestyle alone will not be enough to reduce your cholesterol, so you will also need to take medication.
-Eat a healthy balanced diet that is low in saturated fat
-plenty of fresh fruit and vegetables
-Keeping fit and active will also help to keep your heart healthy and it’s essential that you don’t smoke.
-If you have FH, a healthy lifestyle alone will not be enough to reduce your cholesterol, so you will also need to take medication.
Can I get tested for it
-Go to your doctor to have your cholesterol checked. If a close relative has had a heart attack at a young age (before 55 in a man and before 65 in a woman), then it’s important that you do this.
If your doctor considers that you may have FH, he or she should refer you to a specialist for an assessment, which is likely to include gene tests. The specialist will explain which of your relatives should be checked out, too.
-Go to your doctor to have your cholesterol checked. If a close relative has had a heart attack at a young age (before 55 in a man and before 65 in a woman), then it’s important that you do this.
If your doctor considers that you may have FH, he or she should refer you to a specialist for an assessment, which is likely to include gene tests. The specialist will explain which of your relatives should be checked out, too.
Gene puzzle
There are three genes in which we know mutations (a permanent change in the DNA sequence) can cause FH. When we look at those three genes in people with FH, we can find mutations in about 80 per cent of cases. We are now looking at what is going on in the other 20 per cent. It may be that there is another gene to find.
It’s an exciting possibility that, if we find a new gene in which defects cause high cholesterol, we could develop a new drug to treat it. In 2003, scientists found the third gene in which mutations cause FH. Less than ten years later, a drug that targets the protein made by this gene is being trialled and seems to be effective in lowering cholesterol in both FH and non-FH patients. It is hoped that it may be
There are three genes in which we know mutations (a permanent change in the DNA sequence) can cause FH. When we look at those three genes in people with FH, we can find mutations in about 80 per cent of cases. We are now looking at what is going on in the other 20 per cent. It may be that there is another gene to find.
It’s an exciting possibility that, if we find a new gene in which defects cause high cholesterol, we could develop a new drug to treat it. In 2003, scientists found the third gene in which mutations cause FH. Less than ten years later, a drug that targets the protein made by this gene is being trialled and seems to be effective in lowering cholesterol in both FH and non-FH patients. It is hoped that it may be
What does treatment involve?
FH can be easily and effectively treated with a cholesterol-lowering statin. A high-intensity statin such as atorvastatin or rosuvastatin is needed to bring it down. Sometimes a different cholesterol-lowering drug called ezetimibe is given as well as a statin. Regular follow-up appointments are important, too. Lifestyle changes (see What can I do, above) can also reduce your risk of heart disease.
How is it inherited?
FH can be easily and effectively treated with a cholesterol-lowering statin.FH is caused by changes in one of three genes. Genes are the DNA instructions that our body uses to tell every cell how things should function.
The genes involved in FH tell the body to produce proteins that are involved in clearing LDL cholesterol – the harmful type of cholesterol – from the bloodstream. So if one of them is faulty, then your body won’t get the correct instructions.
If someone carries a faulty gene – and therefore has FH – then there is a 50:50 chance that they will pass it on to each of their children.
FH can be easily and effectively treated with a cholesterol-lowering statin. A high-intensity statin such as atorvastatin or rosuvastatin is needed to bring it down. Sometimes a different cholesterol-lowering drug called ezetimibe is given as well as a statin. Regular follow-up appointments are important, too. Lifestyle changes (see What can I do, above) can also reduce your risk of heart disease.
How is it inherited?
FH can be easily and effectively treated with a cholesterol-lowering statin.FH is caused by changes in one of three genes. Genes are the DNA instructions that our body uses to tell every cell how things should function.
The genes involved in FH tell the body to produce proteins that are involved in clearing LDL cholesterol – the harmful type of cholesterol – from the bloodstream. So if one of them is faulty, then your body won’t get the correct instructions.
If someone carries a faulty gene – and therefore has FH – then there is a 50:50 chance that they will pass it on to each of their children.